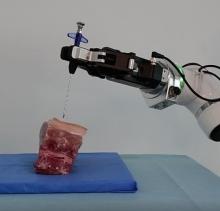
Articulated robotic arm for assistance in interventional radiology
Robotic technology has helped medicine to reduce exposure time and offer greater efficiency and precision in surgical interventions. The goal of using an articulated robotic arm for X-ray (Rx) guided minimally invasive surgery and interventional assistance is to reduce direct and secondary radiation on physicians. The use of a collaborative robotic arm (COBOT) that replaces the operating arm of the surgeon-interventionist physician to avoid exposure to X-rays is described.